Forum Replies Created
-
AuthorPosts
-
Robert GreggParticipantHi Ron,
Excellent case management.
No need for ELMA as you adjust your distance to tissue based on patient response You want them to feel some warmth at first. Gives you and the patient some feedback.
Spend more time–say around 3-5 minutes. Be patient, be thorough, be done with it!
Bob
AnonymousSpectatorBob,
Re:greater distance / more time
My question then is if least amount of energy to get the job done is the ideal , why not use the EMLA and decrease the time? (I understand further distance will affect how much energy is absorbed- so in this case how do you calculate which way is really using the ‘least energy’?)
Thanks,
jetsfanSpectatorI have been lurking for a while and enjoying the posts but I do have several questions regarding anesthesia. Hopefully someone can answer them:
1) 5.25 W 90/90 defocused, how close or how far to the tooth is defocused?
2) Is this setting only for posterior teeth or will it work buccal and lingual of anterior teeth?
3) What if the occlusal surface is mostly amalgam or composite for that matter, where do you aim the tip?
4) after you begin the prep, what settings do you use if patient feels pain and you have entered dentin?
5)I have also heard of anesthesia being achieved using 1.5W buccally and lingually. Anyone use this ? with success? and what settings?
6) I primarily use tapered tips, do I need to lower the 5.25W for anesthesia?
7) HOW BOUT DEM JETS!
AnonymousSpectatorWelcome to the forum! I’ll try and answer your questions below.
5.25 W 90/90 defocused, how close or how far to the tooth is defocused?
I stay far enough away that the laser isn’t marking or altering tooth surface.
Is this setting only for posterior teeth or will it work buccal and lingual of anterior teeth?
I use it both ant and posterior but in the anterior I may adjust downward depending on how deep a restoration I’m doing
What if the occlusal surface is mostly amalgam or composite for that matter, where do you aim the tip
I go right thru the composite .amalgam you need to avoid so you don’t fry a tip
after you begin the prep, what settings do you use if patient feels pain and you have entered dentin?
This is where magnification is so important, soon as the enamel is gone I drop down to 2.5 or lower depending on the patient. I think some of the others may drop to about 3.25
I have also heard of anesthesia being achieved using 1.5W buccally and lingually. Anyone use this ? with success? and what settings?
I think Bill Chen is doing this, in my hands I never got enough anesthetic effect to remove amalgams but he evidently is successful with it
I primarily use tapered tips, do I need to lower the 5.25W for anesthesia?
I don’t for the anesthesia part but do for the prepping
HOW BOUT DEM JETS!
didn’t know Winipeg still had a hockey team

PatricioSpectatorJetsfan,
Good luck from a DNS Packer backer
1. I am a learner so let the buyer beware! I use a defocus distance which is as close as I can get to the tooth without altering the tooth surface. Approximately 1 to 1 1/2 centimeters. In the anterior I generally use 1.5W preset as a start( workd well for me) just because of the reduced amount of water spray. Same guidelines. I go back and use more watts if there is sensitivity when I begin to remove hard tissue. In most cases when I enter dentin and there is sensitivity I go immediately to the small round bur and clean the deeper areas rarely with any patient discomfort. If I need better access I either reintroduce the laser or use the electirc handpiece, again, with rare patient sensitivity and finally I finish with the laser usually at 1.5w to prep the surface and steilize the prep and remove any remaining stain or possible decay. This works well for me. I intend to try Glenn’s method and use a fissuratomy bur to open the intitial entry on the occlusal of molars. The process works on any tooth though I have had less success with second molars. I routinely numb teeth where I intend to remove an amalgam so amalgam is not a problem. The tip is aimed at the cervical area buccal or lingual primarily but I cover as much of the tooth as possible.
Access dictates.With some sensitivity I either start over with the defocused laser, continue preping with a round bur(usual), reduce the watts to 3w or 3.5w or just anesthetize the patient with the ligajet or the big one.
I use the tappered tips also.
Pat
Janet CenturySpectatorNo photos, but I used the diode for the first time to treat an aphthous ulcer – on my significant other / guinea pig. Got to him on the first day and the next day it was GONE. I think this will be a great service to the patients, especially on the little kids who absolutely stop eating when they get one of these.
jetsfanSpectatorthanks for the quick feedback.
J
E
T
S
JETS, JETS, JETS(USA)
Glenn van AsSpectatorHi Jets fan……….I leave the defocussed stuff to Mark and Ron to tell you from the Biolase standpoint but today I did one with the erbium on an anterior tooth at around 4.8 watts (30 Hz and 160 mj ) at a distance of around 1.5 to 2 inches . (Its tough to tell under the scope) for 60 secs.
Lots of water and lots of air………..then went into the composite and patient felt Zero…….
Check out the erbium section I will post the photos.
Glenn
Glenn van AsSpectatorHi Janet……..use both lasers ( the diode works deeper and the erbium more superficial) and I would use the erbium first which is less sensitive and then go deeper but lets see what others suggest.
glenn
Glenn van AsSpectatorHi folks: here is a case I did yesterday, a single veneer/three quarter crown with the argon laser for tissue troughing. I wanted to show you how nice the lateral displacement is once the Expasyl goes in and how it pushes the margin of the tissue away so the lab can see the margin.
The other central already has a veneer on it ………he wanted a pair of front teeth for Xmas………just like the song.
Note the displacement and the pictures of the impression.
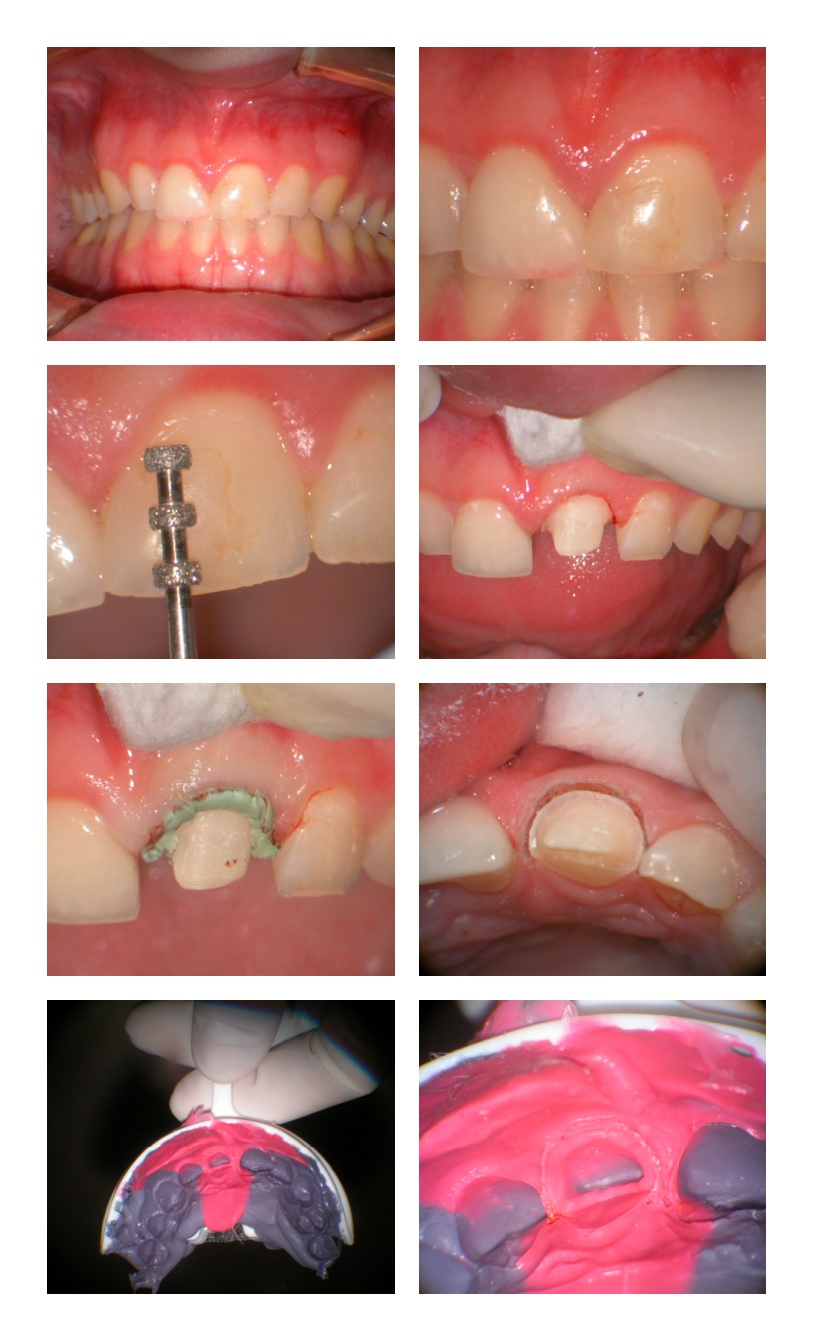
Glenn
2thlaserSpectatorGreat stuff Glenn. Do you always use Expansyl after using laser to trough?
Mark
whitertthSpectatornice stuff glenn.. I too use expasyl after i trough with the laser….they work great together…..
Glenn van AsSpectatorHi Mark…….welcome back and happy new year.
Nah I dont do expasyl all the time…….in anterior cases where I am worried about recession I may do moderate retraction with laser and augment lateral displacement with expasyl.
In posterior teeth, I use the laser more.If Ron is doing this its gotta be great huh!!
Thanks for the kind words guys………….
Glenn
jetsfanSpectatorYesterday I had a young woman with extreme ypersensitivity on a #29. At .25W 0/0 I couldn’t get within an inch of the tooth. I held the tip outside the mouth , retracted the lip and attempted to apply laser energy in a very defocused mode. At that distance it was difficukt to tell if I was aimed at the correct part of the tooth, but she was able to tell me. I eventually anesthestized, lasered area and placed duraphat.
I also have one other patient who has the most severe hypersensitivity post perio treatment that I ever saw.
I attempted desensitizing teeth during my training session with zero success. After reading many posts online I have subsequently attempted treatment also with zero sucess.
These were two failures, I have had several sucess stories, but when I hear people talk of 100% sucess it makes me wonder.
Comments and sugestions appreciated.
GO JETS!
PatricioSpectatorJetsfan,
I think we need to defer to Bob for the best explanation. My only comment is,” perfection is in heaven”. I have had people I could not touch without local and so I go quicly to it. I never promise no discomfort I state what most people experience and ask them to let me know if the laser is bothering them. Some people(I get the feeling )just want to be anesthetized. Any discomfort is too much. I wonder how your second case could eat or drink with such sensitivity. Is it possibly a fear of any dentist pain? The ligajet is a big help for sensitive teeth needing restorations. See John Kanca’s website for his routine. The site is found in one of my posts under hard tissue- anesthesia I believe. Let’s see what the big boys say.
Pat -
AuthorPosts
